A Cavitary Conundrum
Authors: Dylan L McCreary1,2, Lisa Jarnagin2, Daniel Puebla2
1 – University of Arizona College of Medicine Phoenix
2 – Banner University Medical Center Phoenix
Case
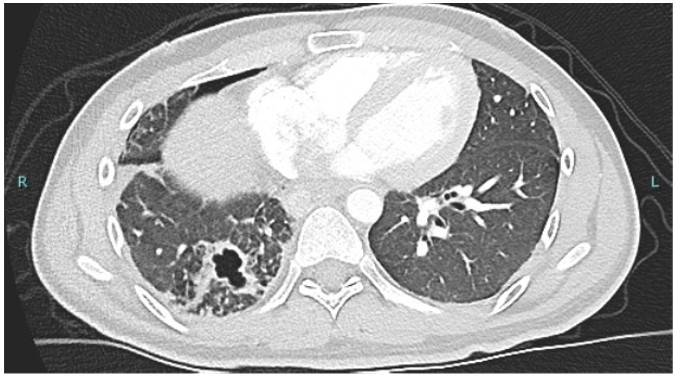
A 27-year-old male with history of diabetes mellitus and pulmonary coccidiomycosis presented to the hospital with hemoptysis and a right lower lobe cavitary lesion. He later developed a right pneumothorax with bronchopleural fistula and underwent a thoracotomy with right lower lobe lobectomy. Pathology from the lobectomy section showed fungal elements forming hyphae like structures in addition to spherules. Laboratory workup showed positive Coccidioides PCR with complement fixation at titer of 1:8. Aspergillus galactomannan antigen in bronchoalveolar lavage specimen and serum beta-D glucan assay were negative.
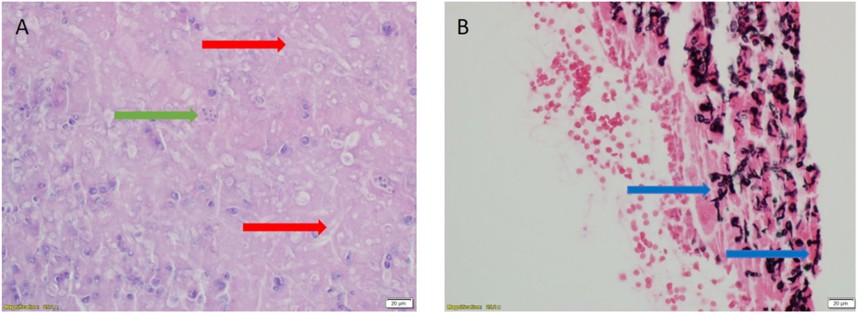
Figure 2: Histopathology section from cavitary lung lesion with H&E stain (Panel A) and GMS stain (Panel B)
Question
What is the most probable cause of the cavitary lung lesion?
- Aspergillus
- Coccidioides
- Aspergillus and Coccidioides co-infection
- Mucor
- Fusarium spp
B. Coccidioides
Discussion
Both Coccidioides and aspergillus may cause cavitary lung disease, but the clinical syndrome above is most consistent with Coccidioides. While Coccidioides most commonly presents in the yeast form (spherules), hyphae like arthroconidia can be found in pathologic specimens as well. The negative aspergillus galactomannan antigen and beta-D-glucan assay reduce the likelihood of aspergillus co-infection and make Coccidioides infection more likely.
Coccidioides is a dimorphic fungus endemic to the Southwestern United States that has significantly increased in prevalence and geographic spread due to multiple factors including climate change, improved diagnosis, and increased rates of immune suppression. Due to this rise it is increasingly important for all clinicians to be familiar with clinical manifestations, diagnosis, and treatment. Infection is usually asymptomatic or causes mild respiratory symptoms, however in the presence of decreased host immune response Coccidioides can cause cavitary lung lesions and disseminated disease. In these settings PCR testing with complement fixation is the gold standard for diagnosis. In certain cases, tissue pathology is obtained, however diagnosis based on tissue pathology alone can be challenging due to the multiple morphologic forms that can be seen in Coccidioides infection.
The hyphae like arthroconidia found in the environment are inhaled into the lungs and form the large circular Coccidioides spherules that are typically isolated from pathologic specimens. These spherules are identified as large spherical structures filled with small circular endospores and are pathognomonic for Coccidioides infection. However, in chronic and atypical infections, such as described in our case, the branched hyphae of the arthroconidia can be isolated. The presence of branched hyphae in a cavitary lesion caused by Coccidioides presents a significant diagnostic challenge due to the morphologic similarity to branching invasive fungi such as Aspergillus, Mucor, and Fusarium. This atypical presentation has been previously documented in multiple studies highlighting the importance of keeping Coccidioides infection on your differential diagnosis even if spherules are not seen. In such cases serologic testing including PCR and complement fixation is crucial to differentiate between these invasive fungal infections and make an accurate diagnosis.
Cultures for the diagnosis of Coccidioides are a specific (reported specificity > 90%), but not sensitive test (sensitivity reported 40-70%). In many cases definitive diagnosis relies upon serum antigen analysis with PCR and complement fixation, which shows sensitivity of 50-80% and specificity 90-96%. Laboratory evaluation of aspergillus includes galactomannan antigen detection (specificity 80% and sensitivity 80%) and beta-d glucan (specificity 85% and sensitivity 77%). In our case the combined results of positive Coccidioides culture and PCR with complement fixation, negative galactomannan and beta-D glucan make the diagnosis of Coccidioides more likely.
In our case the hyphae like structures in the pathologic specimen led to a misdiagnosis of aspergillus infection exposing the patient to potential toxicity from voriconazole. Review of the pathologic specimen in addition to serologic testing results led to appropriate diagnosis of Coccidioides infection with isolation of the atypical arthroconidia form on pathology. It is crucial that clinicians are aware of the atypical forms of Coccidioides infection including the branch like hyphae of the arthroconidia form to avoid misdiagnosis and inappropriate treatment. In cases where pathologic diagnosis is uncertain serologic testing for Coccidioides including PCR with complement fixation should be used to guide diagnosis.
References
-
Bays DJ, Thompson GR 3rd. Coccidioidomycosis. Infect Dis Clin North Am. 2021 Jun;35(2):453-469
-
Crum NF. Coccidioidomycosis: A Contemporary Review. Infect Dis Ther. 2022 Apr;11(2):713-742
-
Kassis C, Durkin M, Holbrook E, Myers R, Wheat L. Advances in Diagnosis of Progressive Pulmonary and Disseminated Coccidioidomycosis. Clin Infect Dis. 2021 Mar 15;72(6):968-975
-
Brennan-Krohn T, Yoon E, Nishino M, Kirby JE, Riedel S. Arthroconidia in lung tissue: an unusual histopathological finding in pulmonary coccidioidomycosis. Hum Pathol. 2018 Jan;71:55-59
-
Nosanchuk JD, Snedeker J, Nosanchuk JS. Arthroconidia in coccidioidoma: case report and literature review. Int J Infect Dis. 1998 Jul-Sep;3(1):32-5